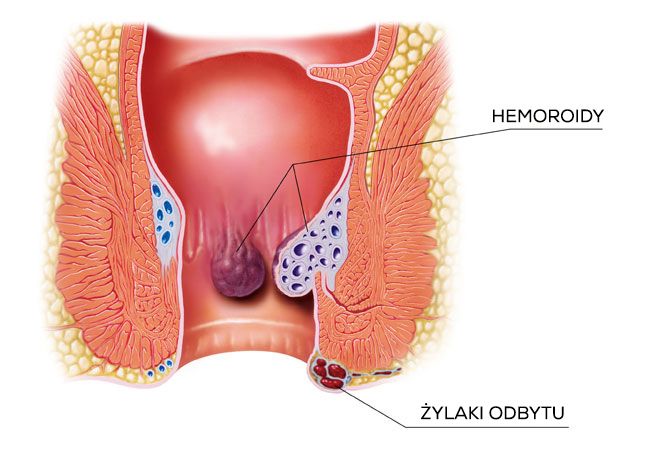
Everyone has haemorrhoids, which are also referred to as piles or varicose veins of anus. All people, including even small children, have haemorrhoids as they are normal anatomical structures. The notion ‘haemorrhoid’ originates from Greek (αἱμορροΐς). It is a combination of the following words: blood - haema and flow - rhoos.
In fact, haemorrhoids are cavernous bodies which resemble cushions filled with blood. They are posterior arteriovenous anastomoses. Physiologically, haemorrhoids are located above the so called dentate line of anus. It ensures their proper functioning. They also support sphincter complex of anus which prevents from uncontrollable flatulence.
dr Maciej Chwaliński
Lorem ipsum dolor sit amet, consectetur adipisicing elit, sed do eiusmod tempor incididunt ut labore et dolore magna aliqua. Ut enim ad minim veniam, quis nostrud exercitation ullamco laboris nisi ut aliquip ex ea commodo consequat.
Disease description

Enlarged hemorrhoids are one of the most common health problems in the population.

Hemorrhoids affect 85% of pregnant women.
Based on the progression, haemorrhoids may be classified into four grades:
I - haemorrhoids do not prolapse the anal canal
II - haemorrhoids reside inside the anal canal and they are visible under anoscopy
III - haemorrhoids are visible outside the anus with straining
IV - haemorrhoids are always outside the anal canal and they are not reversible
Constantly enlarged haemorrhoids cannot be put back inside the anal canal. It is associated with symptoms which are experienced by a patient to a lager extent. A list of the most common symptoms includes bleeding, burning sensation in the anal area, itching and pain. In this case, we refer to the so called haemorrhoidal disease.
The first stage of haemorrhoidal disease consists in a slight bleeding or feeling a discomfort in the anal area.
Haemorrhoids, which are examined by the proctologist using speculum, bulge but do not prolapse. Successive stages are accompanied by the prolapse of haemorrhoids with straining. Manual reduction of haemorrhoids brings some relief over time. Large haemorrhoids protruding from the anal canal, which are not reversible and are always outside the anus, belong to the most problematic ones. If enlarged haemorrhoids are not treated, they gradually become larger. Consequently, symptoms become more intense over time and more invasive methods of treatment must be applied.
Important issues
Is haemorrhoidal disease a prevalent health condition?
Similarly to venous insufficiency of lower extremities, haemorrhoidal disease is one of the most prevalent health conditions in the present times.
Similarly to venous insufficiency of lower extremities, haemorrhoidal disease is one of the most prevalent health conditions in the present times. It is estimated that even more than 50% of the population in highly developed countries have problems with enlarged haemorrhoids.
How is haemorrhoidal disease diagnosed?
Surgeon-proctologist makes a diagnosis of haemorrhoidal disease. During the examination, haemorrhoids may be visible or palpable on per rectum exam. Examination with a speculum called anoscope or rectoscope is carried out when a special instrument is inserted into the rectum as to allow for the inspection of the anal canal and rectum and visualization of lesions.
Surgeon-proctologist makes a diagnosis of haemorrhoidal disease. During the examination, haemorrhoids may be visible or palpable on per rectum exam. Examination with a speculum called anoscope or rectoscope is carried out when a special instrument is inserted into the rectum as to allow for the inspection of the anal canal and rectum and visualization of lesions.
Although haemorrhoidal disease is one of the most prevalent conditions of posterior parts of intestine, other rare ailments such as fissures or fistulas in the anal area as well as the thrombosis of rectal venous plexus should not be forgotten. Thus, consultation with surgeon-proctologist is required while qualifying for the method of treatment. Avoidance of examination and treatment often result in a deterioration in the condition of the patient or delay in making an appropriate diagnosis.
Who is most commonly diagnosed with haemorrhoidal disease?
The prevalence of haemorrhoidal disease increases with age. It occurs rarely in individuals aged less than 20-25 years.
The prevalence of haemorrhoidal disease increases with age. It occurs rarely in individuals aged less than 20-25 years. Besides genetic factors, which are of significance in some patients, pregnant women are also at higher risk of developing haemorrhoidal disease, especially those that delivered a child more than twice. Haemorrhoidal disease is more common in obese people, those who lift heavy objects, sit for long periods of time, have problems with defecation or suffer from enteritis.
Problems with blood flow and venostasis in the area of anus and rectum may also occur in people with neoplasm of large intestine or other tumours of small pelvis as well as people with disorders in hepatic portal vein circulation and hypertension in abdominal veins.
What are the minimally invasive methods used for the treatment of enlarged haemorrhoids?
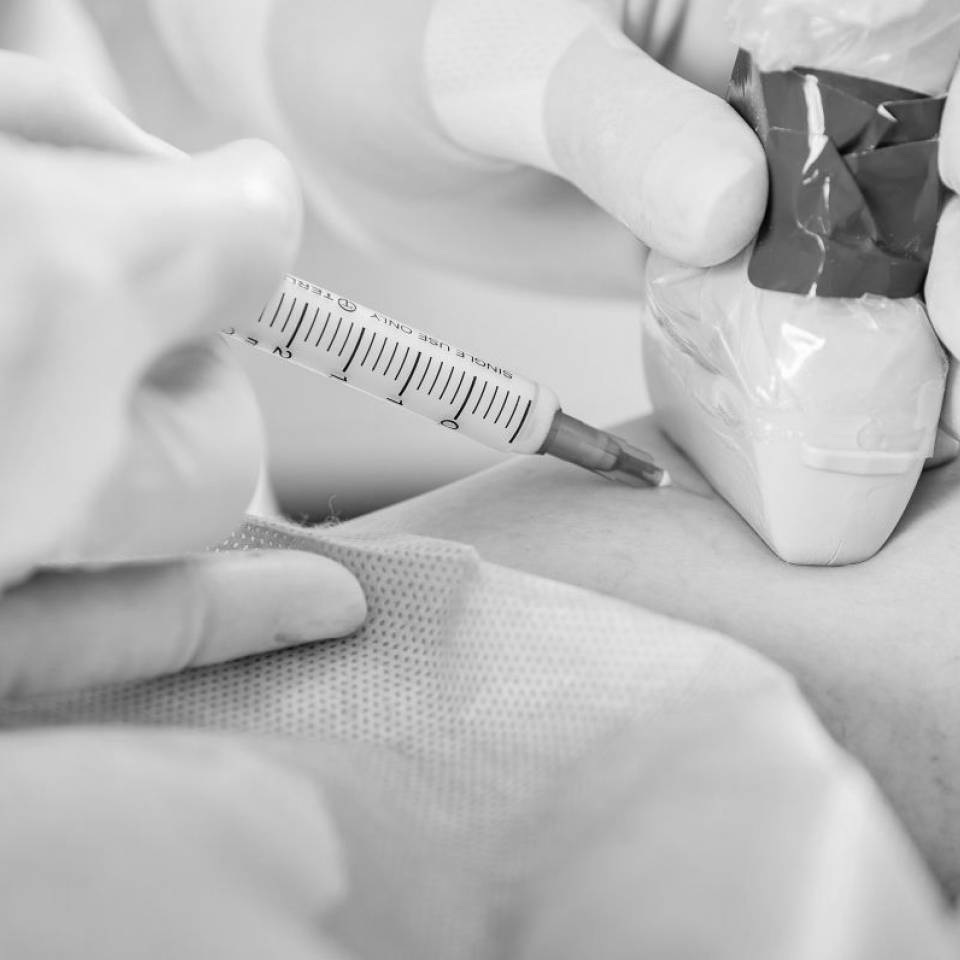
Conservative approach (dietary changes and phlebotropic drugs) and surgical approach are used in the therapy of enlarged haemorrhoids. Nowadays, new minimally invasive methods are more commonly used. Due to an increased awareness, patients who suspect haemorrhoidal disease seek medical advice earlier when the disease is less advanced.
Conservative approach (dietary changes and phlebotropic drugs) and surgical approach are used in the therapy of enlarged haemorrhoids. Nowadays, new minimally invasive methods are more commonly used. Due to an increased awareness, patients who suspect haemorrhoidal disease seek medical advice earlier when the disease is less advanced.
Currently, older minimally invasive methods such as sclerotherapy, Barron’s ligation ("banding"), Hemoron or Oberon methods are replaced by modern procedures.
In the Phlebology Clinic, two minimally invasive methods are used to reduce haemorrhoids:
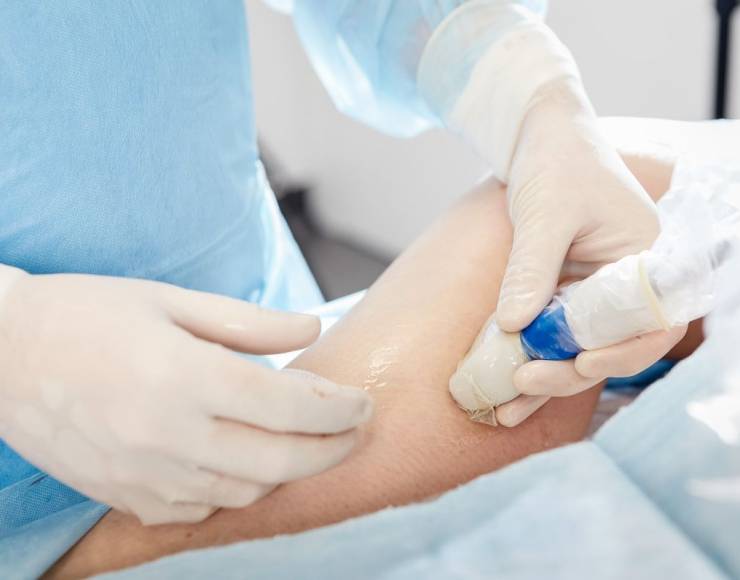
- laser-based method Laser HemorrhoidoPlasty (LHP, ELVeS system)
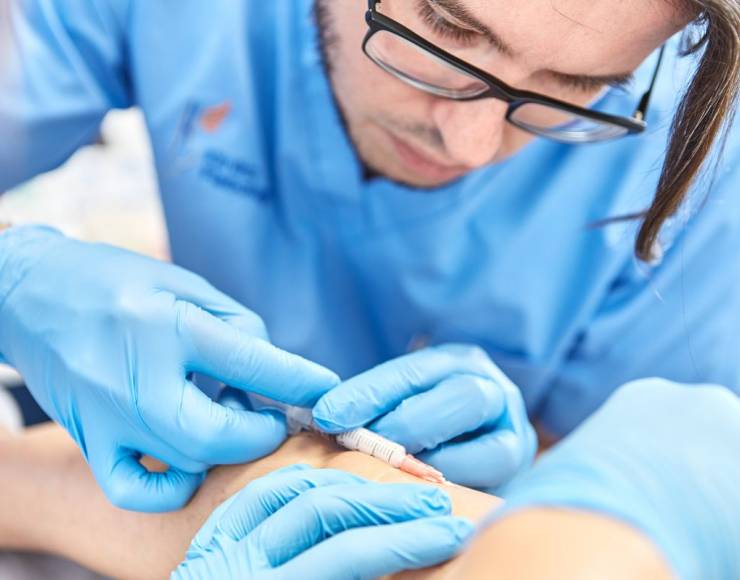
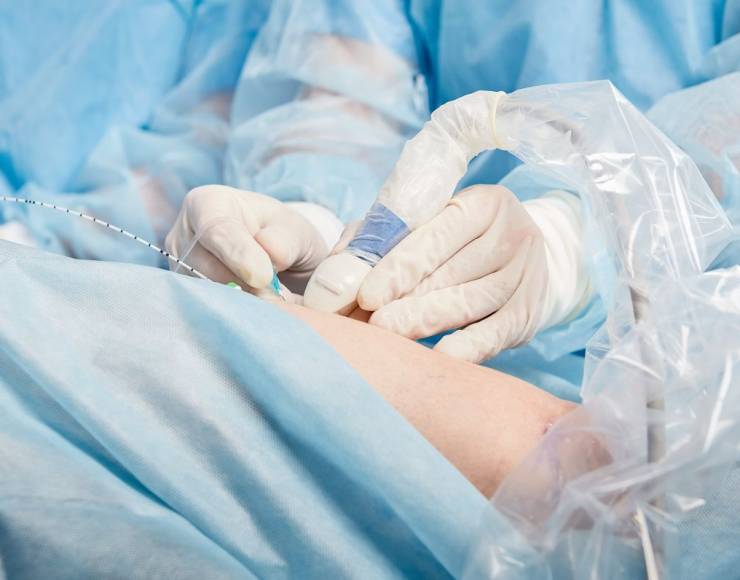
- Doppler-Guided Hemorrhoidal Artery Ligation (DG HAL)
What is the characteristics of varicose veins of anus?
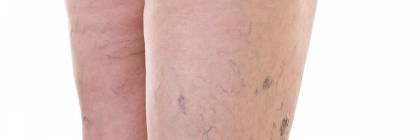
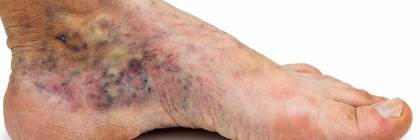
Varicose veins of anus are different from the enlarged haemorrhoids. The part of our body the so called rectal venous plexus contributes to the occurrence of varicose veins of anus. Contrary to haemorrhoids which are identified with ‘internal haemorrhoids’, varicose veins of anus are sometimes referred to as ‘external haemorrhoids’. Inflammation and thrombosis accompanied by redness and swelling around the anus are the most common diseases of rectal venous plexuses.
Varicose veins of anus are different from the enlarged haemorrhoids. The part of our body the so called rectal venous plexus contributes to the occurrence of varicose veins of anus. Contrary to haemorrhoids which are identified with ‘internal haemorrhoids’, varicose veins of anus are sometimes referred to as ‘external haemorrhoids’. Inflammation and thrombosis accompanied by redness and swelling around the anus are the most common diseases of rectal venous plexuses.
Conservative approach, e.g. sitz bath, suppositories, ointments and surgical approach, e.g. excision and evacuation of the clot may be adopted in the treatment of the thrombosis of rectal venous plexus. Proctologist makes the decision on the method of treatment.
Methods of treatment
Testimonials
 dr n. med. Cezary Szary
dr n. med. Cezary Szary

konsultacja flebologiczna z USG Doppler
Jestem bardzo zadowolona z wizyty. Zarówno podczas badania jak i po, zostało mi wszystko dokładnie opisane i wytłumaczone. Dr bardzo uprzejmy i dzieli się swoją wiedzą i......
Czytaj więcej
 Zespół Kliniki Flebologii
Zespół Kliniki Flebologii

Zdecydowanie polecam. Jestem po zabiegu. Naprawdę bezboleśnie. Fachowa opieka. Teraz czekam na końcowy efekt, bo pierwsze zmiany na lepsze są widoczne od razu. Super......
Czytaj więcej
 Dr hab. n. med. Tomasz Grzela
Dr hab. n. med. Tomasz Grzela

laserowe usuwanie żylaków
Dr Tomasz Grzela to wspaniały lekarz. Jestem 3 m-ce po zabiegu laserowym, niestety także chirurgiczny oraz skleroterapii. Wszystko wygojone. Jestem spokojna. Nogi eleganckie :) Teraz tylko kontrole...
Czytaj więcej
 dr n. med. Justyna Wilczko-Kucharska
dr n. med. Justyna Wilczko-Kucharska

konsultacja flebologiczna
Wspaniała Pani Doktor Wilczko. Profesjonalne podejście. Piękne......
Czytaj więcej
 dr n. med. Justyna Wilczko-Kucharska
dr n. med. Justyna Wilczko-Kucharska

konsultacja flebologiczna
Bardzo profesionalne a zarazem cieple przyjecie/powitanie. Fachowa obsluga z pewnym opisem mozliwosci/opcji leczenia(jesli jest wymagane). Bardzo dziekuje. Very professional and yet warm welcome and...
Czytaj więcej
 dr n. med. Cezary Szary
dr n. med. Cezary Szary

wizyta konsultacyjna
Pełny profesjonalizm. Fachowo podchodzi do klientki.Pełna diagnostyka z poradą.Nie naciągacz. Jako jedyny zdiagnozował żylaki odbytu które są przyczyną żylaków kończyn dolnych. Polecam z pełną...
 Dr hab. n. med. Tomasz Grzela
Dr hab. n. med. Tomasz Grzela

konsultacja flebologiczna z USG Doppler
Pierwsza wizyta - bardzo dobre wrażenie. Szczegółowe badanie, jasne i precyzyjnie wyjaśnienia, wysoka kultura osobista. Bez problemu uzyskałam też dodatkowe wyjaśnienia już po wizycie, za...
Czytaj więcej
 dr n. med. Cezary Szary
dr n. med. Cezary Szary
zamknięcie żylaków kończyn dolnych
Drugim etapem leczenia było zamknięcie żylaków kończyn dolnych metodą skleroterapii. Zabieg polega na zamknięciu żył a następnie po ich wygojeniu na usunięciu krwi która w nich pozostała. Szybkie...
Czytaj więcej
 dr n. med. Cezary Szary
dr n. med. Cezary Szary

konsultacja flebologiczna z USG Doppler
5+ dla Pana doktora Doktora! Dr Cezary Szary -To Wspaniały lekarz, polecam w 100%. Bardzo żałuję że tak późno trafiłam do Pana Doktora- bo gdybym wcześniej się do Niego zgłosiła może już...
Czytaj więcej
 Dr hab. n. med. Tomasz Grzela
Dr hab. n. med. Tomasz Grzela

Doktor Tomasz Grzela jest świetnym chirurgiem i flebologiem. W praktyce stosuje nie tylko najnowsze metody, ale etykietę lekarską z wyższej półki. Nie dawno odbyłam dwa zabiegi, z których jestem...
Czytaj więcej
 dr n. med. Cezary Szary
dr n. med. Cezary Szary

wizyta konsultacyjna
Kompetentny, miły, uprzejmy, bardzo dobry specjalista, który ma dobry kontakt z pacjentem. Potrafi wytłumaczyć, na czym polega schorzenie i metodę leczenia. Godny zaufania i......
Czytaj więcej
 dr Dominika Plucińska
dr Dominika Plucińska

konsultacja flebologiczna
Mega profesjonalne i miłe podejście Pani doktor, miła obsługa na......
Czytaj więcej
 Dr hab. n. med. Tomasz Grzela
Dr hab. n. med. Tomasz Grzela

konsultacja flebologiczna z USG Doppler
Byłam bardzo zadowolona z konsultacji. Pan doktor zrobił USG obu nóg, jedną zakwalifikował do dalszego leczenia, druga okazała się w porządku, co było pewną ulgą. Zaproponował różne możliwości...
Czytaj więcej
 dr n. med. Cezary Szary
dr n. med. Cezary Szary

konsultacja flebologiczna z USG Doppler
Byłam u dr. Szarego na USG - Doppler żył po zakrzepicy. Doktor badanie wykonał niezwykle dokładnie, komentując co widzi i co z tego dla mnie wynika. Przejrzał badania wcześniejsze i również się do...
Czytaj więcej
 dr n. med. Justyna Wilczko-Kucharska
dr n. med. Justyna Wilczko-Kucharska

zabieg usuwania żylaków
Bardzo profesjonalna i mila Pani Doktor. Od wielu lat cierpiałam na poważne żylaki. Dzięki Pani Doktor pozbyłam się bólu nóg, który był ddla mnie bardzo uciążliwy. Na początku miałam...
Czytaj więcej
 Dr hab. n. med. Tomasz Grzela
Dr hab. n. med. Tomasz Grzela

wizyta konsultacyjna
Wszystko ok, dokładne badanie, jasne zalecenia. Pan doktor jest bardzo miły i profesjonalny.......
Czytaj więcej
 dr n. med. Cezary Szary
dr n. med. Cezary Szary

USG Doppler żył
Byłam u dr. Szarego na USD - Doppler żył po zakrzepicy. Doktor badanie wykonał niezwykle dokładnie, komentując co widzi i co z tego dla mnie wynika. Przejrzał badania wcześniejsze i również się do...
Czytaj więcej
 Zespół Kliniki Flebologii
Zespół Kliniki Flebologii

konsultacja flebologiczna
Bardzo profesjonalne i dokładne badanie, Pani Anna klarownie mi wyjaśniła wyniki badania i podała odpowiednią metodę leczenia, czas rekonwalescencji oraz metody zapobiegania rozwoju dolegliwości. Bardzo...
Czytaj więcej
 dr n. med. Cezary Szary
dr n. med. Cezary Szary
leczenie żylaków po ciąży
Jeśli chodzi o dr. Szarego nie mogę napisać w kilku słowach. ... Przede wszystkim lekarz z powołania, bardzo kompetentny .Zależy mu by wyleczyć pacjenta a nie tylko zaleczyc. Szuka przyczyny problemu a...
Czytaj więcej